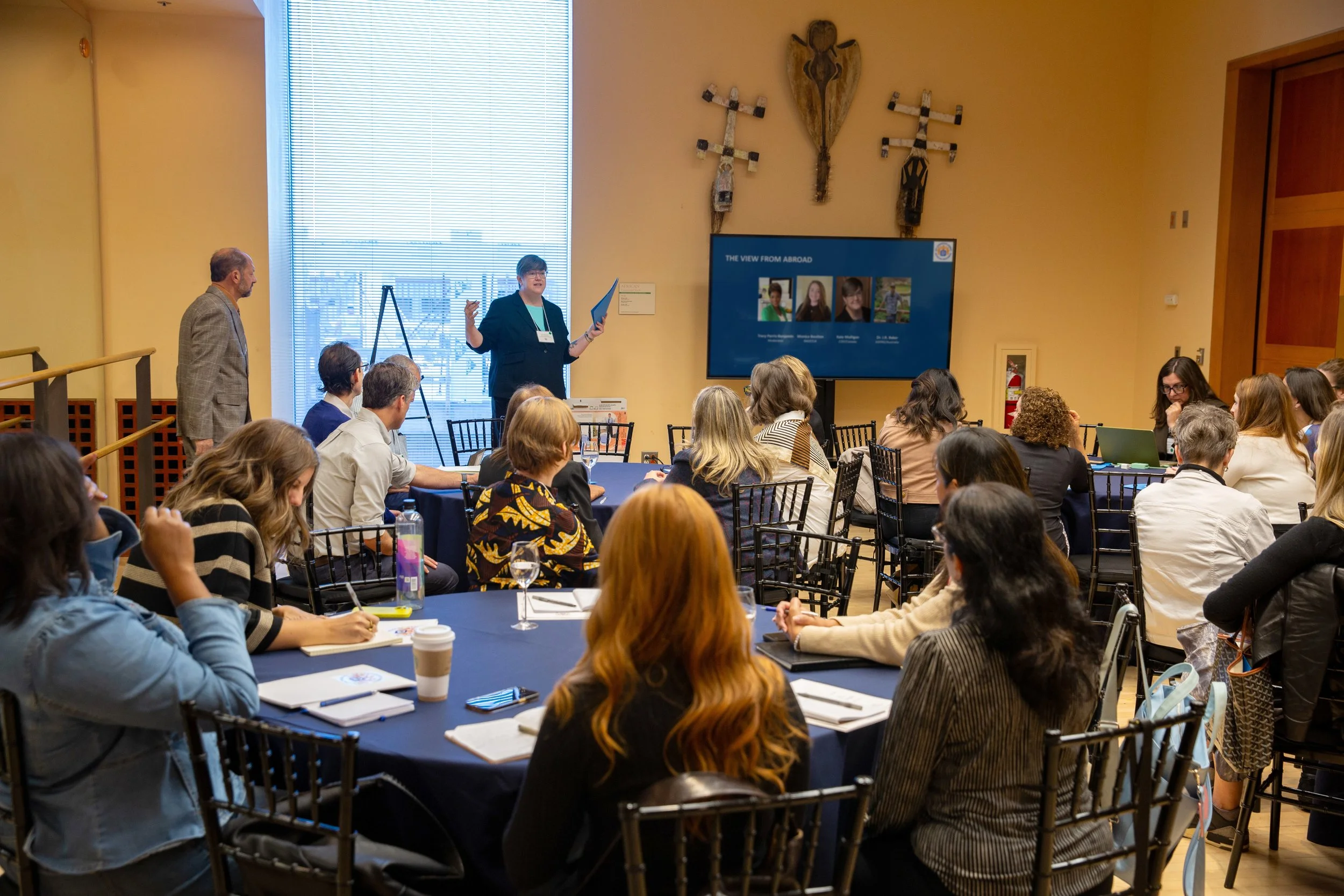
A Report from the First U.S. Social Prescribing Leadership Summit
October 17, 2025
Building the Future of Social Prescribing in the United States
Over the past few years, the global social prescribing movement has made significant strides in the United States. Substantial media attention on the practice from around the world, increased recognition of the loneliness epidemic by public and medical officials—particularly after the COVID-19 pandemic—and numerous new studies and reports on the health benefits of social connection have driven strong interest in social prescribing across the country among medical professionals and citizens alike.
In recognition of this momentum, on October 17, 2025, Social Prescribing USA, the leading national advocacy organization for social prescribing in the United States, organized the inaugural US Social Prescribing Leadership Summit in Newark, New Jersey. The Summit brought together approximately 50 national leaders to identify key priorities for advocates and implementers to rally around, increase coordination and alignment between efforts, and set the stage for the next phase of the movement in the United States.
The following is a summary of the Summit. Download the full report for a complete overview.
We are thankful to the Laurie M. Tisch Illumination Fund for its lead funding of the Summit. We are also thankful to Resonance Philanthropies for its significant support of the gathering. The Benjamin Goldberg Foundation, Connecting through Music Foundation, and multiple private funders also supported the Summit.
Photos and videos by Kieran McConville.


Throughout the summit, participants identified critical areas requiring coordinated action to realize the potential of social prescribing in the United States:
1. Research & Evidence
Build a Strong Evidence Base
Participants emphasized the urgent need to collect and mobilize evidence demonstrating the impact of social prescribing on health outcomes, healthcare utilization, and cost reduction.
Establish Standardized Measures
The group identified the critical need for universal measurement frameworks that allow programs to be compared and findings to be aggregated.
Support Mixed-Methods Approaches
Participants advocated for research that combines quantitative data with storytelling and qualitative insights.

2. Financial Sustainability
Identify Diverse Funding Streams
Participants explored multiple pathways to sustainable funding, including Medicaid 1115 waivers, Medicare Advantage programs, rural health transformation grants, employer wellness initiatives, and integrated mental health funding.
Integrate with Existing Healthcare Payment Models
Discussion centered on working within current healthcare systems, including developing appropriate billing codes, demonstrating return on investment to payers, and aligning social prescribing with value-based care arrangements.
Support Link Worker Infrastructure in the U.S. Context
Clear definition and sustainable funding for the link worker role was identified as essential. Participants recognized that the link worker role, so critical to social prescribing systems in the United Kingdom and elsewhere, would need to be adapted for the United States context.

3. Communications
Increase Public and Provider Understanding
A major barrier identified was the lack of awareness about social prescribing among both the general public and healthcare professionals, despite increased focus on the subject.
Define Clear Standards and Language
The group emphasized the importance of aligned terminology, shared frameworks, and consistent language.
Tailor Messaging by Audience
Different stakeholders respond to different framings of social prescribing. Effective communication requires understanding what matters most to each audience and adapting the message accordingly.

4. Building on What's Working
Leaders discussed leveraging advances and interest in currently popular healthcare efforts and platforms to promote and advance social prescribing in the United States. These efforts include aligning with federal, state, and local initiatives addressing the following priorities:
Arts and Health
The first US Social Prescribing Leadership Summit was held at New Jersey Performing Arts Center (NJPAC) at the conclusion of the Creating Healthy Communities Convening. That event brought together 500 people from across the United States who are thinking, working, and innovating at the intersections of arts and culture, public health, and community development. It is clear that the energy and rapid growth of arts prescribing efforts can benefit all social prescribing efforts in the United States through research and visibility.
Social Connection/Social Health
As health systems, communities, and individuals seek more effective ways to improve wellbeing and prevent chronic disease, enhancing social connection and social health through social prescribing efforts is gaining recognition as a powerful, low-cost, and human-centered contributor to health that supports resilience, healing, and quality of life across the lifespan. Leaders from the Foundation for Social Connection participated in the Summit and have been coordinating many key efforts in this area.
Lifestyle Medicine
The increased interest and expansion of lifestyle medicine—health interventions and practices that use everyday habits such as healthy eating, physical activity, sleep, stress management, and other healthy behaviors to prevent, treat, or improve chronic disease—holds promise as a platform to integrate social prescribing. Key physicians associated with the American College of Lifestyle Medicine participated in the Summit.
Social Determinants of Health
Social prescribing efforts have much to learn from and build on efforts to integrate Social Determinants/Drivers of Health (SDOH) screenings and related interventions into medical care. The Social Interventions Research and Evaluation Network (SIREN) at UCSF participated in the Summit as did key social prescribing leaders from the U.K., Canada and Australia that emphasize social drivers of health within their social prescribing systems.
What Social Prescribing USA Can Do
As a growing national advocacy organization that serves as a significant voice for the collective efforts of the social prescribing movement in the United States, Social Prescribing USA asked gathered leaders how the organization could best serve the movement. Participants challenged Social Prescribing USA to step up in several key ways:

Facilitate Leadership Gatherings
Leaders asked Social Prescribing USA to organize future gatherings at both the national and regional levels to advance the collective social prescribing movement and foster collaboration rather than competition.

Establish Working Groups
Social Prescribing USA was asked to develop working groups on priority topics, including research standards, training and certification, policy development, and technology integration. These groups would bring together experts to develop shared resources and advance specific initiatives.

Develop a Centralized Evidence Repository
Social Prescribing USA was challenged to build and maintain an accessible library of research evidence, measurement tools, implementation guides, and best practices that can serve as a resource for organizations launching or scaling social prescribing programs.

Create Educational Resources
Participants asked Social Prescribing USA to develop practical tools, including playbooks for speaking with healthcare leadership, guides for billing and reimbursement, training materials for link workers, and resources for community organizations serving as referral partners.

Build Strategic Partnerships
Social Prescribing USA was encouraged to develop collaborations with national health organizations, including primary care associations, health system councils, community health worker networks, and organizations that serve older adults and youth.

Looking Forward

The US Social Prescribing Leadership Summit represented a critical inflection point for the movement. With growing awareness of the loneliness epidemic, increasing recognition of social determinants of health, and demonstrated public interest in non-pharmaceutical approaches to wellbeing, conditions are favorable for social prescribing to flourish in the United States.
The path forward requires simultaneous action on multiple fronts: building the evidence base, creating sustainable funding models, establishing training and credentialing systems, developing supportive policies, and—perhaps most importantly—fostering the collaborative relationships that will allow the movement to thrive.
As participants emphasized throughout the Summit, social prescribing is fundamentally about relationships: between patients and providers, between healthcare and community organizations, and between individuals and their communities. The strength of those relationships will determine the success of social prescribing in improving health and wellbeing across the United States.

